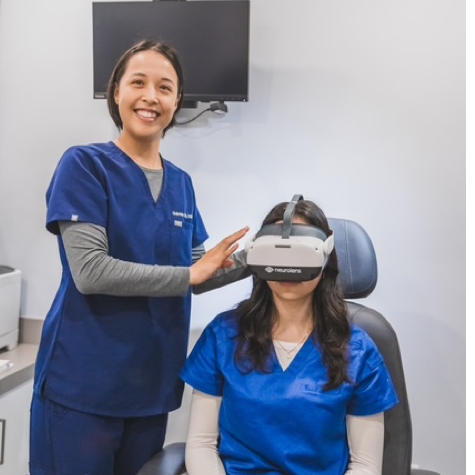
You rub your eyes constantly, reach for eye drops multiple times a day, and still feel like sand is stuck under your eyelids. When dry eye symptoms persist despite your efforts to find relief, the problem might run deeper than you think.
Autoimmune conditions can attack the glands that produce tears, leading to chronic dry eye that requires specialized treatment beyond standard eye drops. When your immune system mistakenly targets healthy tissue in your eyes, you need a comprehensive approach to manage both the symptoms and the underlying cause.
How Autoimmune Conditions Trigger Dry Eye
Your immune system normally protects you from harmful bacteria and viruses. When autoimmune conditions develop, this protective system gets confused and begins attacking your body’s own healthy tissues. The small glands around your eyes that produce tears often become targets in this process.
Inflammation from autoimmune activity reduces both the quality and quantity of your tears. Your tear film becomes unstable, leaving dry patches on your eye surface that feel scratchy and uncomfortable. Over time, chronic inflammation can permanently damage these tear-producing glands.
Common Autoimmune Conditions That Affect the Eyes
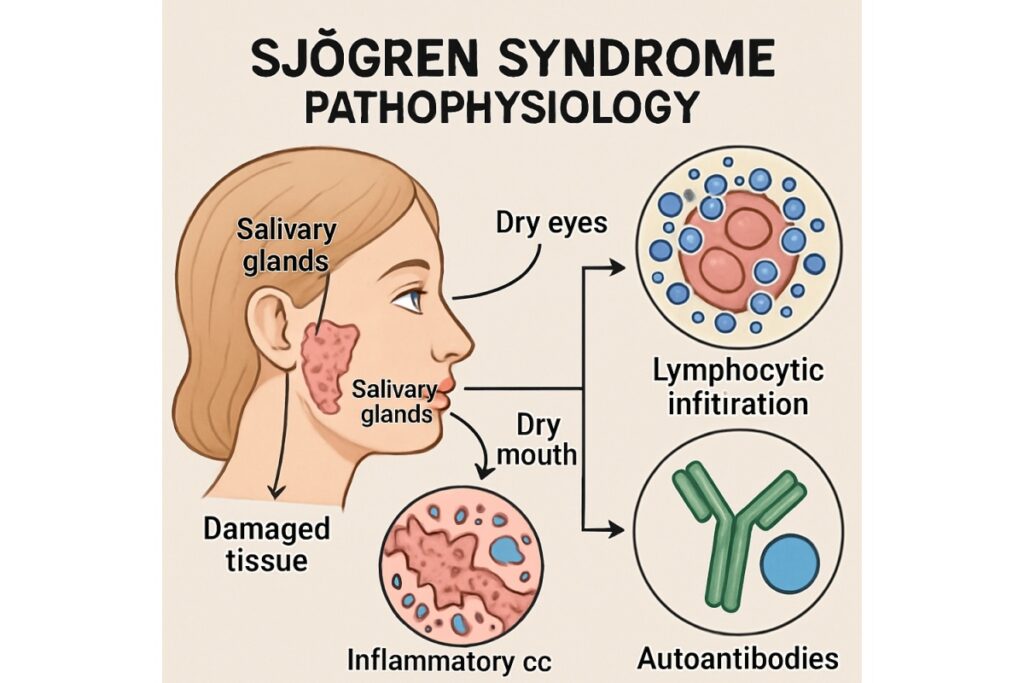
Sjögren’s syndrome targets the glands that produce tears and saliva. You might notice your mouth feels dry while your eyes become uncomfortable. The condition affects millions of people, with women experiencing it more frequently than men.
Rheumatoid arthritis doesn’t just affect your joints; it can also inflame the tissues around your eyes. If you already manage joint pain and stiffness, dry eye symptoms might indicate your condition is affecting other parts of your body.
Lupus creates widespread inflammation that can impact multiple organ systems, including your eyes. The autoimmune activity in lupus often affects the tear glands and the delicate skin around your eyelids. Understanding these connections helps you recognize when your dry eye condition might need specialized autoimmune treatment.
Signs Your Dry Eye Might Be Autoimmune-Related
Regular artificial tears provide temporary relief for most cases of dry eye. When you use eye drops consistently but still experience persistent dryness, burning, or irritation, autoimmune activity might be the underlying cause.
Signs of Potential Autoimmune Involvement
- Systemic physical symptoms: Joint pain, morning stiffness, and general fatigue, along with dry eye, often suggest an overactive immune system.
- The “Sicca” connection: Experiencing dry mouth in combination with dry eye is a primary indicator for specific autoimmune conditions, such as Sjögren’s syndrome.
- Glandular impact: When these symptoms occur together, it highlights a clear link between immune system dysfunction and the body’s moisture-producing glands.
When to See Your Optometrist
Schedule an appointment when dry eye symptoms interfere with reading, computer work, or driving. These daily activities require clear, comfortable vision, which can be difficult when your tear film isn’t working properly.
Professional comprehensive eye exams can detect subtle changes in your tear production and eye surface health that indicate autoimmune involvement.
How Your Optometrist Diagnoses Autoimmune Dry Eye
A comprehensive dry eye evaluation identifies both the type of dry eye you have and its underlying cause. Dr. Zargar Eyecare uses advanced diagnostic technology to assess your tear production, tear quality, and eye surface health.
Your assessment may include:
Tear Production & Quality Tests:
- Schirmer test: Measures how much natural tears your eyes produce over a set period
- Tear breakup time (TBUT): Uses special dye to show how quickly your tear film evaporates between blinks
- Osmolarity testing: Measures salt concentration in your tears, which increases with dry eye disease
Inflammation & Surface Damage Detection:
- MMP-9 test: Detects inflammatory markers on your eye surface that indicate immune system activity
- Fluorescein staining: Highlights areas of surface damage or dryness not visible during routine examination
Meibomian Gland Assessment:
- LipiScan imaging: Captures detailed images of your meibomian glands to evaluate their health and function
- Meibomian Gland Evaluator (MGE): Applies gentle pressure to assess oil gland secretions and detect blockages
- LipiView tear film analysis: Evaluates the lipid (oil) layer of your tear film
Because autoimmune conditions often cause systemic symptoms alongside dry eye, your optometrist will ask about joint pain, dry mouth, skin changes, and family history of autoimmune disease. This medical history helps connect your eye symptoms to potential autoimmune involvement and guides treatment recommendations.
When Additional Testing Is Needed
If your dry eye evaluation reveals signs of autoimmune involvement—such as severe aqueous deficiency, positive inflammation markers, or symptoms like dry mouth and joint pain—your optometrist may refer you to a rheumatologist for further testing.
A rheumatologist can order blood tests to detect autoimmune markers such as:
- Antinuclear antibodies (ANA)
- SSA/SSB antibodies (specific to Sjögren’s syndrome)
- Rheumatoid factor
- Other immune system indicators
Salivary flow rate testing may also be performed to assess saliva production. When both tear and saliva production are significantly reduced, these findings support a diagnosis of Sjögren’s syndrome or other autoimmune conditions.
This collaborative approach between your eye doctor and rheumatologist ensures you receive comprehensive care that addresses both your eye symptoms and the underlying autoimmune condition.
Treatment Options for Autoimmune Dry Eye
Prescription anti-inflammatory eye drops target the immune activity that damages your tear glands. These medications help reduce inflammation more effectively than artificial tears alone. You might need to use them consistently for several weeks before noticing improvement.
Punctal plugs are tiny devices that block the drains in your eyelids, helping your natural tears stay on your eye surface longer. This treatment works well when combined with other therapies to manage autoimmune dry eye.
Treatments like intense pulsed light (IPL) therapy can help restore normal function to the glands around your eyelids. These in-office procedures complement your daily eye care routine. Meibomian gland dysfunction often accompanies autoimmune dry eye, and targeted treatments address both the immune system involvement and the mechanical blockage of these important oil glands.
Daily Management Strategies
Moist warm compresses applied to your closed eyelids for 10-15 minutes help improve oil production from the glands along your eyelid margins. The gentle heat makes these oils flow more easily, improving your tear quality.
Humidifiers add moisture to dry indoor air that can worsen your symptoms. This simple addition to your home or office environment helps preserve your natural tears throughout the day.
Long-Term Eye Health with Autoimmune Conditions
Regular monitoring helps catch changes in your condition before they affect your vision. Autoimmune conditions can fluctuate over time, and your eye care needs to adapt accordingly. Consistent follow-up appointments help your doctor adjust treatments as your condition changes.
Coordination between your eye doctor and other healthcare providers helps manage all aspects of your autoimmune condition. This team approach helps manage both your eye symptoms and your overall health.
Protect Your Vision
Early intervention helps slow the progression of autoimmune-related dry eye and protects your long-term eye health. When you address inflammation quickly, you can often prevent permanent damage to your tear-producing glands.
Get Advanced Treatments for Relief with Dr. Zargar Eyecare
Every person with autoimmune conditions experiences different symptoms and responds differently to treatments. Dr. Zargar Eyecare develops personalized treatment plans that address your needs and help you maintain comfortable, clear vision.
Contact us today to schedule a comprehensive evaluation and take the first step toward managing your autoimmune dry eye symptoms.